With one in five adults in the U.S. having been diagnosed with Major Depressive Disorder (MDD), antidepressants, particularly selective serotonin reuptake inhibitors (SSRIs), are widely used. SSRIs stop or delay the body from reabsorbing serotonin, leaving more of it available for the body to use. This regulates mood, but patients don’t see results for an average of two to four weeks. However research found that depression is the failure of neuroplasticity (the brain’s ability to change and adapt), and that SSRIs work partly due to their ability to boost this. Studies found that synaptic density and plasticity were improved with prolonged use of SSRIs. But, this improvement often takes weeks, likely explaining the delay in mood enhancement. SSRIs enhance brain-derived neurotrophic factor (BDNF) gene expression, which encodes the BDNF protein. BDNF regulates synapse functions through its TrkB receptors. The BDNF-TrkB pathway is key in supporting neuroplasticity. Epigenetic changes are observed in depressed patients; methyl groups attach to BDNF histones, inhibiting the gene expression, and there are not enough acetyl groups on its promoters to counteract this. Activating the transcription factor CREB (cAMP response element binding protein) induces BDNF expression by increasing acetylation which could decrease the time it takes to relieve depression symptoms. The potential for harmful side effects due to too much BDNF can be suppressed with inhibitors for protein kinase A (PKA). We propose the intrastriatal injection of engineered mesenchymal stem cells (MSCs) to accelerate neuroplasticity via BDNF in addition to the use of SSRIs.
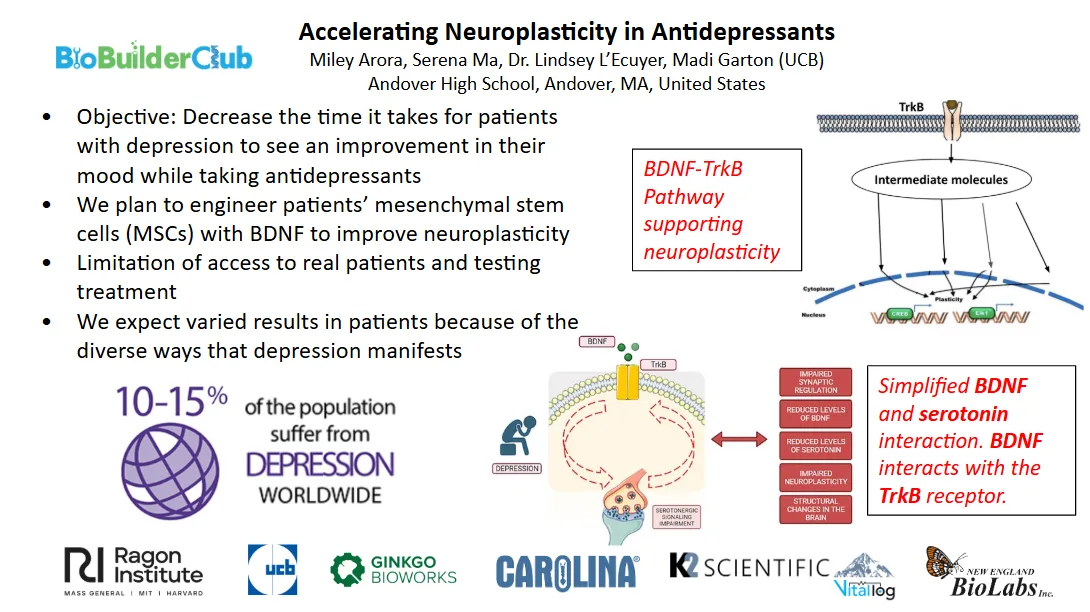
Accelerating Neuroplasticity in Antidepressants
School
Andover High School
Andover, MA
BioBuilderClub Season
2024-2025 Season
Category
Resources
BBC LT_SynapticSculptors_Andover High School_2025
EDITED BBC Poster_SynapticSculptors_Andover High School_2025 (1)